Understanding Tinea Corporis: Causes, Symptoms, Diagnosis, Treatment, and Prevention In English 2024
Introduction
Tinea corporis, commonly known as ringworm, is a fungal infection that affects the skin. Despite its name, it has no relation to worms. This condition is caused by various dermatophyte fungi and can manifest on different parts of the body, leading to distinctive ring-shaped rashes. This comprehensive guide explores the causes, symptoms, diagnosis, treatment options, and preventive measures for tinea corporis.

Causes
Tinea corporis is primarily caused by dermatophyte fungi. These fungi thrive on keratin, a protein found in the outer layer of the skin, hair, and nails. The most common culprits include Trichophyton, Microsporum, and Epidermophyton species. These fungi are highly contagious and can be transmitted through direct contact with infected individuals or by touching contaminated surfaces, such as towels, clothing, or sports equipment.
Symptoms
The symptoms of tinea corporis can vary, but they often include the following:
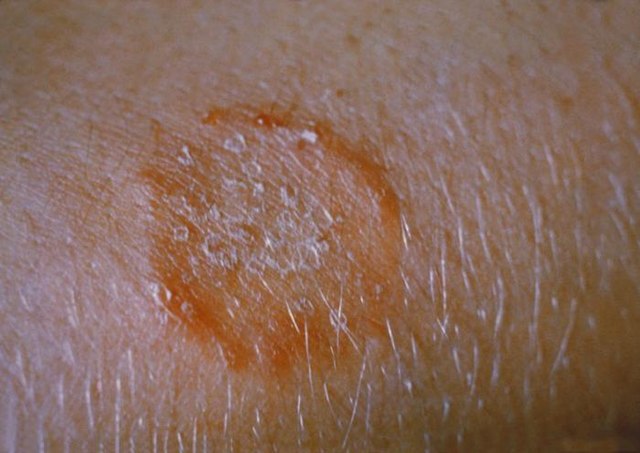
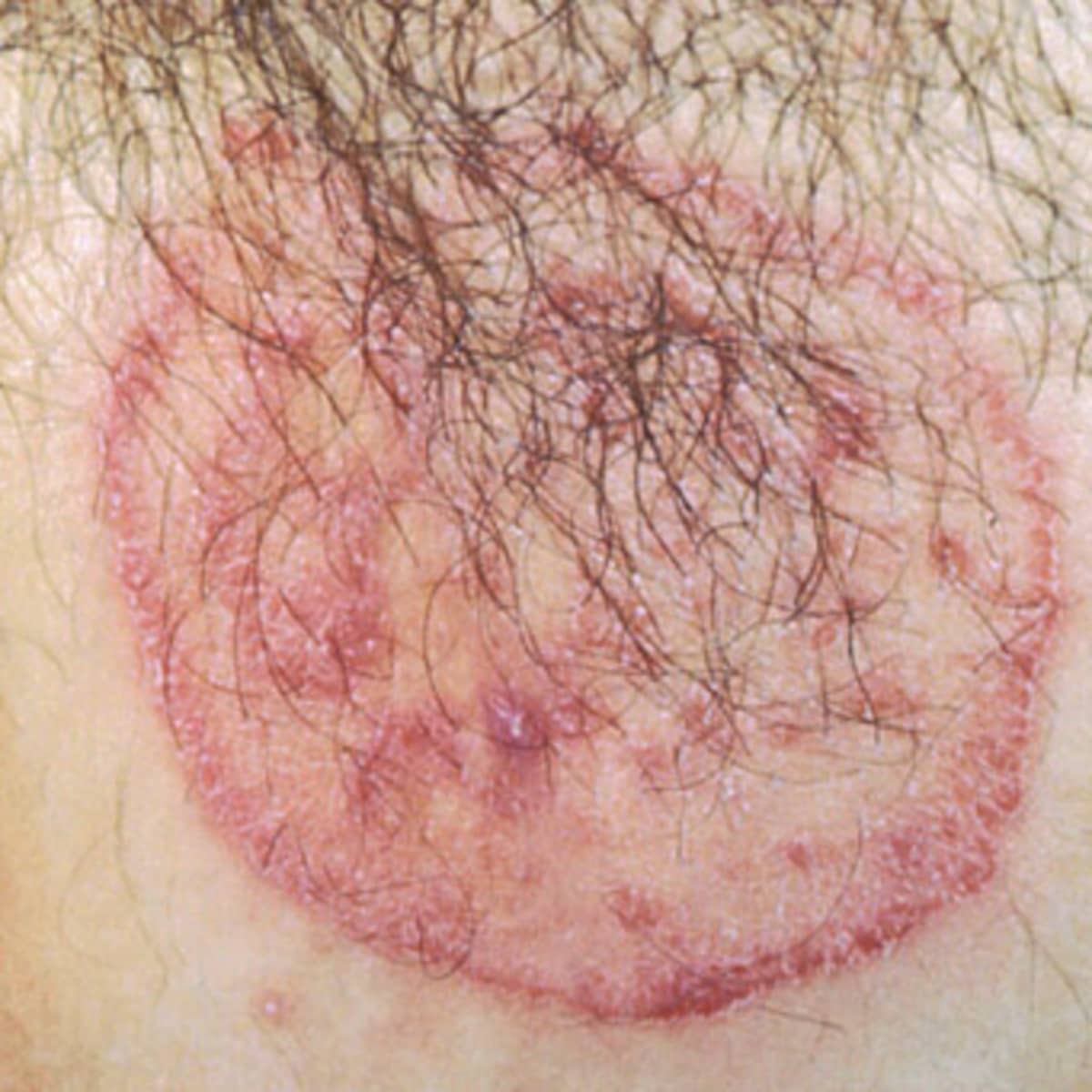
- Circular Rash: One of the hallmark signs of tinea corporis is a raised, red, and circular rash. The center of the rash may appear clearer than the edges, giving it a distinct ring-like appearance.
- Itching: The affected area is usually itchy, and scratching can lead to the spread of the infection to other parts of the body.
- Scaling or Peeling Skin: As the infection progresses, the skin within the ring may become scaly or start to peel.
- Blisters or Pustules: In some cases, tinea corporis may result in the formation of blisters or pustules within the affected area.
- Redness and Inflammation: The skin around the rash may be red and inflamed.
It’s important to note that the appearance of these symptoms can vary depending on the specific type of fungus causing the infection and the individual’s immune response.
Diagnosis
Diagnosing tinea corporis typically involves a combination of clinical examination and laboratory tests. A healthcare professional will examine the rash and may use a Wood’s lamp, a special ultraviolet light, to check for fluorescence, which can indicate the presence of certain fungi. In some cases, a skin scraping or biopsy may be taken and examined under a microscope to identify the specific type of fungus causing the infection.
Treatment
Treatment for tinea corporis often involves antifungal medications, which can be applied topically or taken orally. The choice of treatment depends on the severity of the infection and the specific type of fungus involved.
- Topical Antifungal Creams: Over-the-counter or prescription-strength antifungal creams are commonly used for mild to moderate cases. These creams are applied directly to the affected area and are usually continued for several weeks after the rash has cleared to prevent recurrence.
- Oral Antifungal Medications: For more severe or widespread infections, oral antifungal medications may be prescribed. These medications are taken by mouth and are effective in treating systemic fungal infections.
- Antifungal Powders or Sprays: In some cases, healthcare professionals may recommend antifungal powders or sprays to keep the affected area dry and aid in the healing process.
- Corticosteroid Creams: In cases where there is significant inflammation, corticosteroid creams may be prescribed to reduce redness and itching. However, these should be used under the guidance of a healthcare professional, as they can potentially worsen fungal infections if used inappropriately.
Prevention
Preventing tinea corporis involves adopting good hygiene practices and taking precautions to avoid contact with infected individuals or surfaces. Here are some preventive measures:
- Maintain Good Hygiene: Regular bathing and proper cleaning of the body, especially in areas prone to moisture, can help prevent fungal infections.
- Avoid Sharing Personal Items: Refrain from sharing towels, clothing, or personal items with individuals who have a fungal infection, as this can contribute to the spread of the fungus.
- Keep Skin Dry: Fungi thrive in warm and moist environments. Keeping the skin dry, especially in areas prone to sweating, can help prevent the development of tinea corporis.
- Wear Breathable Clothing: Choose breathable fabrics such as cotton to allow air circulation and reduce the risk of fungal growth.
- Practice Good Foot Hygiene: Keep feet clean and dry, especially between the toes. Use antifungal powders in shoes if necessary.
- Avoid Walking Barefoot in Public Places: Fungi can be present on surfaces like gym floors, swimming pool areas, and communal showers. Wearing sandals or flip-flops in such places can help prevent fungal infections.
- Prompt Treatment of Other Skin Conditions: Promptly treating other skin conditions, such as eczema or psoriasis, can reduce the risk of developing tinea corporis.
Conclusion
Tinea corporis, while not a serious medical condition, can be uncomfortable and unsightly. Understanding its causes, symptoms, and treatment options is crucial for prompt and effective management. If you suspect you have tinea corporis or any other skin condition, it’s essential to consult with a healthcare professional for an accurate diagnosis and appropriate treatment. Additionally, adopting good hygiene practices and preventive measures can go a long way in reducing the risk of fungal infections.
यह पोस्ट हिंदी में पढ़ने के लिए है?
टीनिया कॉर्पोरिस को समझना: कारण, लक्षण, निदान, उपचार और रोकथाम हिंदी में 2024
RELATED KEYWORDS ⬇️
#Tineacorporis
#causesoftineacorporis
#treatmentoftineacorporis
#symptomoftineacorporis



Good
Good
Usesful information
Acha bro